Living Amends
In celebration of World Kidney Day, March 13, we wanted to know: Will organ donations for incarcerated people become a reality in California?
For Central California Women’s Facility (CCWF) resident Maria Serrato, thoughts of freedom are nothing compared to wanting her brother Ricardo to have her kidney. Ricardo is in Stage 4 kidney failure and too far down the donor list to receive the lifesaving care he needs.
When Serrato got the news, she felt “helpless and sad.” Now 57, Serrato was just 22 when she was arrested and left her brother, then 20, behind. Even though their relationship had been strained at times, their family love has not wavered.
Serrato believes that donating her kidney would help the whole family, including her mother. They had many conversations about the donation process. Serrato hoped something could be done — was she a potential match? Could she rescue her brother?
The answer, Serrato eventually found out, is no. According to the California Department of Corrections and Rehabilitation (CDCR) Health Care [sic] Department Operations Manual Section 2.4.1, incarcerated people in California may only choose to donate organs and/or other tissues after death.
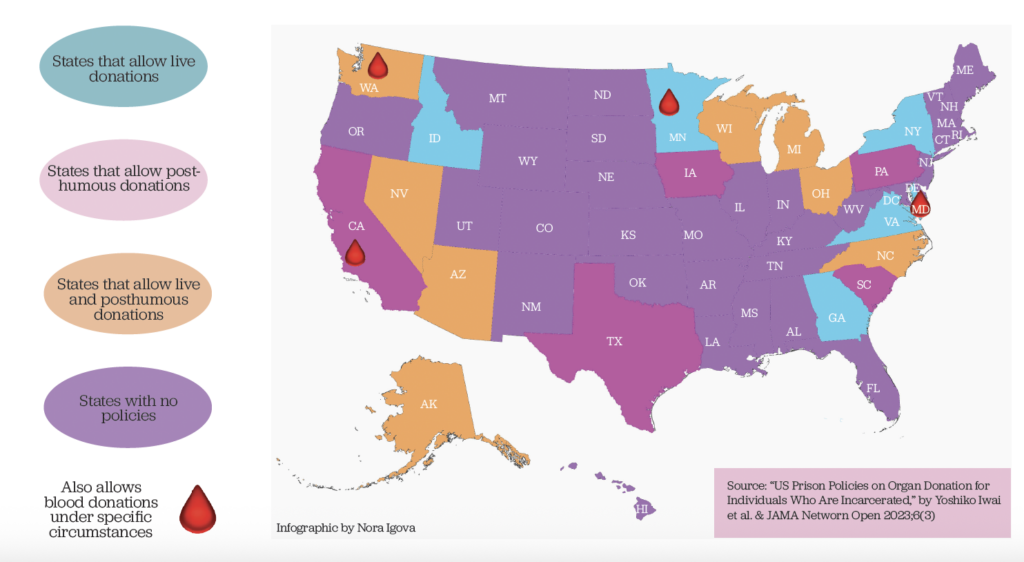
The situation would look a lot different if Serrato were incarcerated in a different state. According to a 2023 article published by the Journal of the American Medical Association (JAMA), 15 state prison systems and the Federal Bureau of Prisons allow incarcerated people to donate organs while living (see the infographic below for state-by-state details).
In states where donation is allowed, regulations vary widely. For example, some states do not allow condemned people to donate. Some allow living donations and others allow only posthumous donations.
In some states, only immediate family members are permitted to receive organs. Minnesota and Washington, where living organ donation is allowed, also permit blood donations. Blood donation is a possibility in California, but only in a case of urgent need.
Organ donation in the free world has been an option since the 1950s. In 1954, Joseph Murray carried out the first successful kidney transplant, according to Austin Sarat, professor of jurisprudence and political science at Amherst College, writing for The Conversation. There has been an urgent demand ever since.
To address that need, Congress passed the National Organ Transplant Act in 1984. This brought a database into play so that individuals in need of an organ could be more effectively matched with donors, and to safeguard against an organ black market.
Alaska became the first state to authorize organ donation by incarcerated persons, in 1986. The most recent policy was written in Arizona, in 2022. According to research published by JAMA, 16 prison systems reviewed and implemented donation policies within the last 10 years, eight of which in the last two years.
The continued pursuit of donors reflects an unrelenting need. In May 2025, the U.S. Health Resources and Services Administration reported there were 103,223 people on the transplant waiting list, with an average of 13 people dying each day for lack of an organ transplant. According to Sarat, racial and ethnic minorities have a particularly challenging time being matched with a donor.
To address the persistent shortage of donors, lawmakers have tried, unsuccessfully, to bring forward other legislation. In California, Senator Cathleen Galgiani (D-Stockton) introduced Senate Bill 1419, called The Uniform Anatomical Gift Act: prison inmates [sic], in February 2016. However, it failed a few months later, in April. The Living Kidney Donor Support Act, introduced in the U.S. Senate in 2023, is still making its way through the legislative process. The bill is supposed to protect existing donors and encourage more donors.
Beyond a lack of legislative will, other concerns complicate green-lighting organ donations from incarcerated persons. These include security issues related to travel outside the prison, the procedure’s cost, and the problem of post-operative duty of care.
The University of California San Francisco’s (UCSF) hospital’s own policies, for example, do not allow incarcerated people to donate organs. It is because, due to their incarceration, they cannot complete a full medical and psychosocial workup, and comply with post-donation follow-up, according to Suzanne Leigh, senior public information representative for the UCSF Office of Communications.
Still, these obstacles have not deterred those willing to donate. Serrato holds out hope of bringing some relief to her brother.
“Every opportunity I have to bring awareness to this problem for incarcerated interested donors is my mission,” she said. “To be of the highest service for Ricardo is my goal.”
But for now, California’s incarcerated persons trying to make amends, the chance to donate an organ will take a while longer to be made into reality.



